Conditions & Treatments

Hysterectomy
In the early 1990’s it was estimated that at least 60% of women presenting with heavy periods would have a hysterectomy to treat the problem, often as a first option. However, things have changed and the number of hysterectomies is decreasing rapidly. A hysterectomy is a big operation that can be associated with complications in a minority of cases. It is also an emotive procedure: because the womb and fertility are often seen as being part of your woman’s identity, the concept can be undesirable for some people.
Nevertheless, clinically, hysterectomy is associated with a very high satisfaction rate by those who have undergone the operation.
Alternative effective treatments to hysterectomy are available for women with heavy periods, particularly for those who have a normal uterus and no significant pathology such as large uterine fibroids. As a result, the hysterectomies now performed tend to be more complicated than many of those in the past.
Types of hysterectomy
There are a various types of hysterectomy. The type you have depends on why you need the operation and how much of your womb and surrounding reproductive system can safely be left in place.
The main types of hysterectomy are:
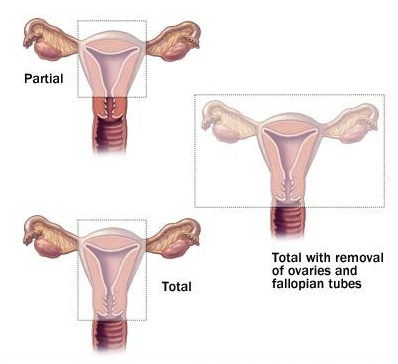
- Total hysterectomy: the womb and cervix (neck of the womb) are removed; this is the most commonly performed operation
- Subtotal hysterectomy: the main body of the womb is removed leaving the cervix in place. Some women are choosing this option to try and protect their pelvic floor from future prolapse
- Total hysterectomy with bilateral salpingo-oophorectomy: the womb, cervix, fallopian tubes (salpingectomy) and the ovaries (oophorectomy) are removed
- Radical hysterectomy: the womb and surrounding tissues are removed, including the fallopian tubes, part of the vagina, ovaries, lymph glands and fatty tissue. This type is reserved for cancer surgery.
There are three ways to carry out a hysterectomy:
- Vaginal hysterectomy: where the womb is removed through a cut in the top of the vagina
- Abdominal hysterectomy: wherethe womb is removed through a cut in the lower abdomen
- Laparoscopic hysterectomy (keyhole surgery): where the womb is removed through several small cuts in the abdomen
Potential complications
Being fit and healthy before you have an operation reduces your risk of developing complications.
As with all types of surgery, a hysterectomy can sometimes lead to complications and some of these are described below:
General anaesthetic
It is very rare for serious complications to occur after having a general anaesthetic (1 in 10,000 anaesthetics given). Serious complications can include nerve damage, an allergic reaction and death (although this very rare; there is a 1 in 100,000 chance of dying after having a general anaesthetic).
Bleeding
As with all major operations, there is a small risk of heavy bleeding (haemorrhage) after having a hysterectomy. If you have a haemorrhage, you may need a blood transfusion (where you receive blood from a donor).
Bladder or bowel damage
In rare cases, damage to abdominal organs, such as the bladder or bowel can occur. This can cause problems, such as infection, incontinence or a frequent need to urinate.
It may be possible to repair any damage during the hysterectomy. You may need a temporary catheter to drain your urine.
Infection
There is always a risk that an infection will develop after any operation. This could be a urinary tract infection, a chest infection or a vaginal infection. These aren't usually serious and can be treated with antibiotics.
Thrombosis
A thrombosis is a blood clot that forms in a vein and interferes with blood circulation and the flow of oxygen around the body. The risk of developing blood clots increases after having operations and periods of immobility. You will be encouraged to start moving around as soon as possible after your operation. You may also be given a blood-thinning medication, such as warfarin, to reduce the risk of clots.
Vaginal problems
If you have a vaginal hysterectomy there is a risk that you will have problems at the top of your vagina where the cervix was removed. This could range from slow wound healing after the operation to prolapse in later years.
Ovary failure
Even if one or both of your ovaries are left intact, they could fail within five years of having your hysterectomy. This is because your ovaries receive some of their blood supply through the womb, which is removed during the operation.
Early menopause
If you have had your ovaries removed, it's likely that you'll have menopausal symptoms, such as hot flushes, sweating, vaginal dryness and disturbed sleep soon after your operation. This is because the menopause is triggered once you stop producing eggs from your ovaries (ovulating). This is an important consideration if you're under the age of 40 because early onset of the menopause can increase your risk of developing brittle bones (osteoporosis). This is because the level of the hormone, oestrogen, decreases during the menopause. Depending on your age and circumstances, you may need to take additional medication to prevent osteoporosis.
Recovering from a hysterectomy
A hysterectomy is a major operation. You can be in hospital for up to five days following surgery and it takes about six to eight weeks to fully recover.
Rest as much as possible during this time and don't lift anything heavy, such as bags of shopping. You need time for your abdominal muscles and tissues to heal.
Surgical menopause
If your ovaries are removed during a hysterectomy, you will go through the menopause immediately after the operation, regardless of your age. This is known as a surgical menopause. If one or both of your ovaries are left intact, there's a chance you will experience the menopause within five years of having your operation.
If you experience a surgical menopause after having a hysterectomy, you should be offered hormone replacement therapy (HRT).




